It’s no secret that America’s COVID vaccine rollout didn’t get off to the greatest start last December. The situation has improved in the ensuing weeks, although large state-by-state disparities remain.
If you’re looking for an analog for the current roadblocks to vaccine distribution, think of the issues which plagued the initial days of coronavirus testing.
From communication issues between the federal and local governments to a glut of the very supplies necessary to administer a vaccine in the first place (such as syringes), there are a multitude of challenges to the most ambitious immunization campaign in more than a century. And many of the troubles are inextricably linked.
Here are the five biggest problems and what we know about them so far.
Allocating COVID vaccines and materials
After doses of Pfizer/BioNTech’s or Moderna’s COVID vaccines have been manufactured, they must make their way to health systems, nursing homes, and pharmacy partners. And any time you have to deliver a product somewhere the “last mile” challenge is inevitable.
Some facilities remain confused about how many doses they’ll be receiving in a given week. Dr. Melanie Swift, who’s helping oversee the rollout process at the Mayo Clinic in Minnesota, describes it as essentially an ad hoc process.
There has also been trouble on the federal front involving vaccine reserves. The Trump administration claimed that there was a large enough reserve of vaccines to serve the needs of states as more and more people qualified to receive one. But after federal recommendations that COVID shots be available for people over 65 in mid-January, states like Washington, New York, and Oregon were left blowing in the wind because the reserves just didn’t exist.
And then there’s the ancillary issue of securing the materials necessary to administer vaccines such as vials and syringes. When you’re attempting to vaccinate hundreds of millions of people in the course of a year, there can be a bottleneck for basic materials, as was the case with COVID testing.
The nascent Biden administration said Wednesday that it had invoked the Defense Production Act (DPA) in order to expedite the manufacturing of such materials, although it’s unclear exactly which firms would be responsible for the manufacturing.
“It was invoked, and it means our work is ongoing with companies to ensure that we are expediting the manufacturing of materials to ensure that we can get 100 million shots in the arms of Americans,” said White House press secretary Jen Psaki.
It’s probably a safe bet that companies which have already been working on creating more syringes and similar products such as Becton Dickinson will be involved in that process in the coming months.
Different states have different COVID strategies
When the Pfizer and Moderna COVID vaccines received Food and Drug Administration (FDA) emergency use authorization (EUA), the Centers for Disease Control (CDC) issued a list of recommendations for who to prioritize.
The key word there is “recommendations.” As former Secretary of Health and Human Services (HHS) Alex Azar made clear in the waning days of the Trump administration, states would ultimately be responsible for determining their own process for rolling out the vaccine.
That’s meant to create flexibility for locales based on their individual needs. But it can also breed confusion and disparate results in vaccination rates.
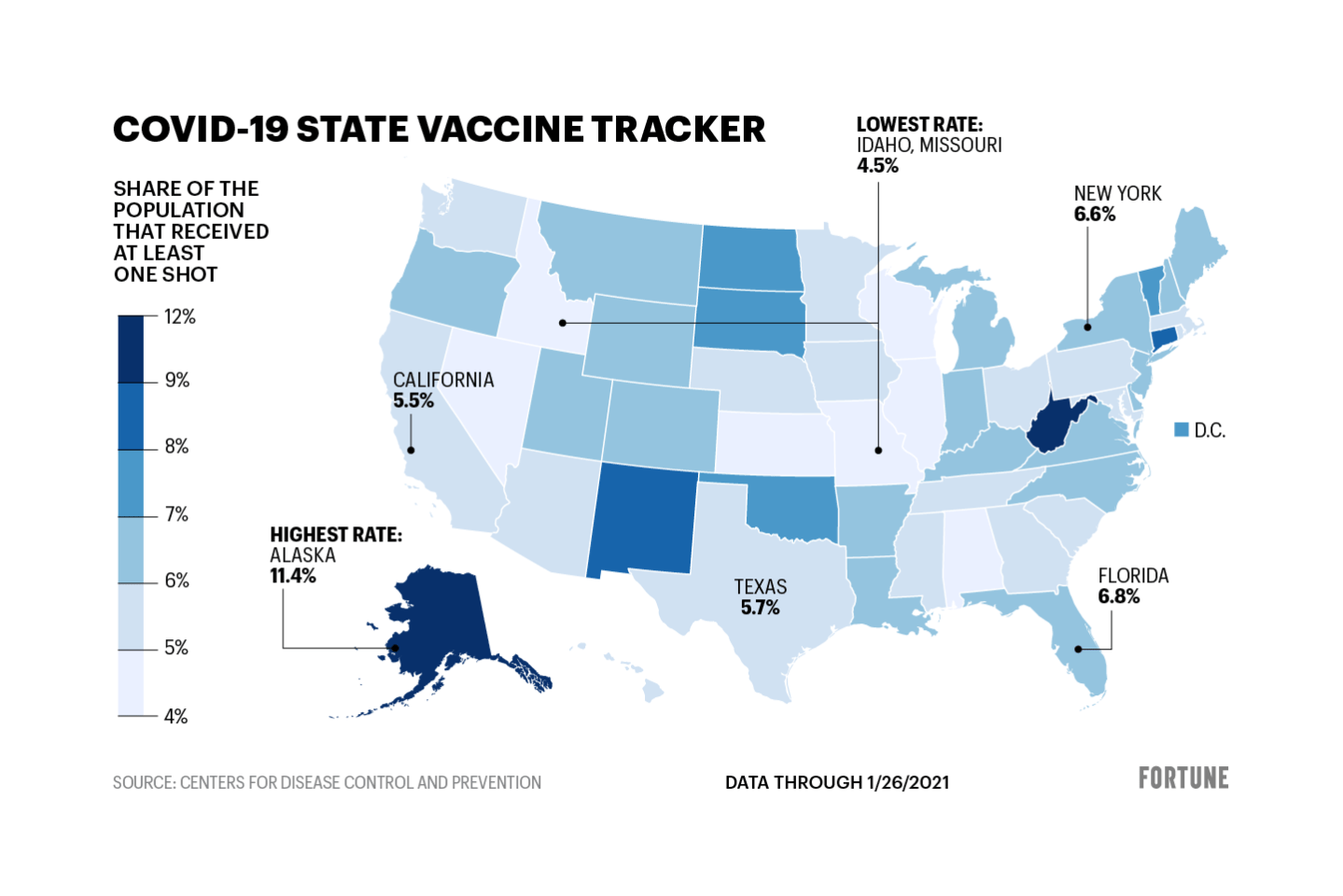
For instance, the percentage of the population who have received at least one dose of the two-dose Pfizer or Moderna vaccines range from lows of 4.5% in Idaho and Missouri to 11.4% in Alaska. Some of that may be explained by different population densities; but divergent policies could play a role, too.
“Overall, we find states are increasingly diverging from CDC guidance and from each other, suggesting that access to COVID-19 vaccines in these first months of the U.S. vaccine campaign may depend a great deal on where one lives,” writes the nonpartisan health care think tank Kaiser Family Foundation (KFF) in a report earlier this month.
“In addition, timelines vary significantly across states, regardless of priority group, resulting in a vaccine roll-out labyrinth across the country.”
Jumping the COVID vaccine line
There are several reasons that the COVID vaccine rollout comes in phases. First, there’s the obvious issue of making sure there’s enough vaccine supply to meet demand. There’s the reality that neither of the vaccines in the U.S. have technically been given full approval yet, just emergency authorization for an extraordinary circumstance. And then there’s the prioritization of the people who would need and benefit from a vaccine the most, much like in the early days of COVID testing.
The first tranches of people who were recommended to get the vaccine included frontline health care workers and long-term care facility and nursing home residents since they are among the highest risk groups for coronavirus. And then came recommendations to expand availability to those over the age of 65. Eventually, more or less all Americans will be eligible.
But there have been numerous reports both in the U.S. and abroad of individuals jumping the line to get a COVID vaccine. This has led to repercussions in some cases, such as a Canadian CEO who resigned his job after it was revealed that he and his wife lied about their occupations to receive the Moderna vaccine.
And therein lies the rub. It can be difficult to verify whether someone truly qualifies for a COVID vaccine or is an essential worker. After all, you don’t have to take your pay stub or tax documents to a vaccination site.
There’s also a practical issue: In some areas, not enough people who do qualify are receiving the vaccine, leading to doses going bad and being tossed in the trash. Health care providers have been hesitant to report the waste numbers out of fear of retribution, according to NBC.
Given that reality, it makes sense that some doctors and facilities would rather give a dose to someone who doesn’t technically qualify yet rather than throw a COVID vaccine into the garbage. But there’s a difference between benefiting from a salvaged dose and deliberately jumping the line.
While public health officials want to see as many people as possible eventually get vaccinated, the chaotic distribution strategy is creating disparities for high-risk people who could use one right now.
People simply not wanting to take a COVID vaccine
If getting a COVID vaccine to where it needs to go is a last mile challenge, then actually getting shots into arms is a last inch challenge. And it’s in part a persuasion dilemma because of COVID vaccine skepticism.
A January survey by the Kaiser Family Foundation found that 20% of those polled say they would either definitely not get the shot or would only do so if mandated. An additional 31% are in a holding pattern to see exactly how effective and safe it is.
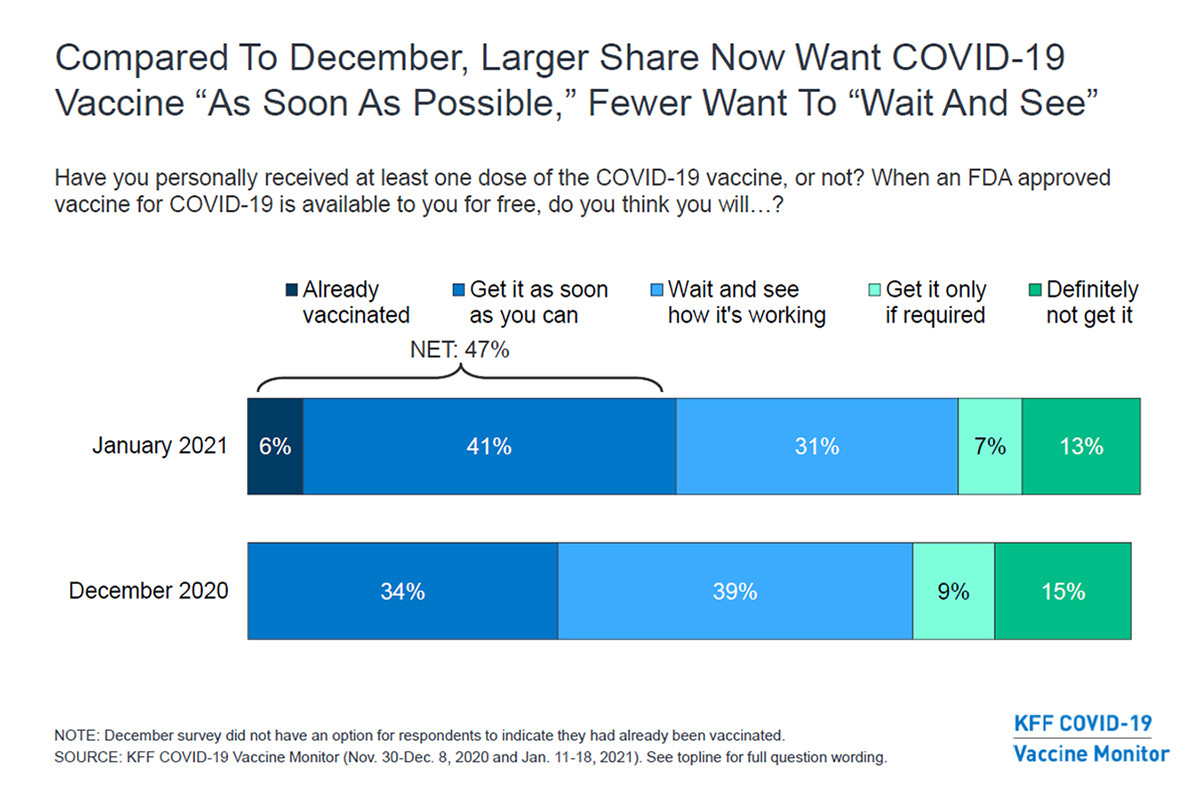
The good news is those are better numbers than December, as Kaiser’s findings show. But ultimately upwards of 70% and even up to 90% of the population will need to be immunized in order to achieve herd immunity against COVID across the nation.
Data communication across the private and public spheres
Tarek Tomes knows a little something about data as the commissioner and chief information officer (CIO) for the state of Minnesota. And he paints the vaccine distribution dilemma as one tightly bound to a data communications problem.
“I think one of big the things that certainly jumps out to me is how unprepared as a country we were and really still are,” he said during an interview on Fortune‘s Brainstorm podcast earlier this month, adding that we must “make sure we invest in the infrastructure related to technology that moves around health information.”
Communication is everything during a pandemic but the systems which are tasked with sharing data are largely outdated and have to grapple with a labyrinth of information. Companies such as electronic health records vendor Epic have had to create ad hoc systems in order to store data on, say, who has been vaccinated for large hospital systems, which itself required coordination between health care providers and medical IT companies.
The trouble is the sheer number of different players involved and the data lag that comes with it. Information about COVID vaccine needs must travel from local hospitals to state governments and the federal government, which must then communicate with manufacturers such as Pfizer and Moderna, drug distributors such as McKesson, logistics firms like UPS and FedEx, pharmacies such as CVS and Walgreens, and, oh, the general public.
The CDC does have a portal for these datasets that’s meant to serve as a more central hub for extremely decentralized coronavirus vaccine information. But it’s still a largely federated process that’s forcing locales to figure out the technologies to communicate their needs in a timely fashion.











