Dear readers—happy Thursday.
I saw a number of articles over the past few days suggesting that there’s a “second wave” in coronavirus cases in certain states like Florida and Texas. But the clear spike in at least nine states isn’t a second wave at all—it’s a continuation of the first one which still hasn’t been quelled.
The terminology of a “second wave” only makes sense if the first has subsided. That’s just the nature of waves. What’s going on right now is more akin to ebbs, flows, and ripples being driven by highly inconsistent reopening strategies.
Take a look at one map from my Fortune colleagues Erika Fry and Nicolas Rapp (keep in mind this is based on one set of consistent methodology and that the numbers may be different depending on exactly which dataset you’re using):
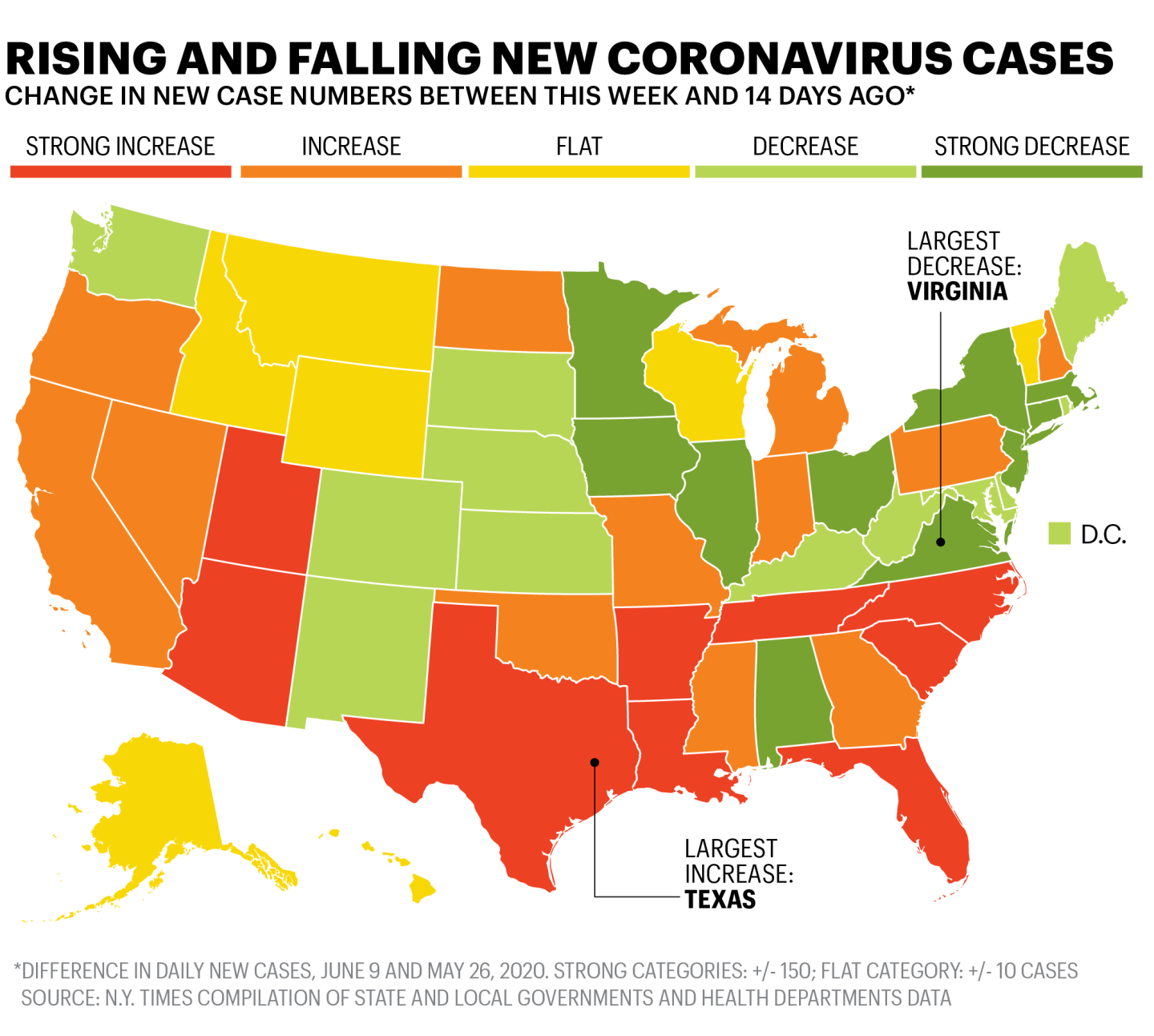
The number of COVID-19 cases and deaths in places like New York, the epicenter of the pandemic, have declined sharply in recent weeks. But public health experts have largely attributed that to an aggressive strategy promoting mask use, social distancing, and restrictions on mass gatherings.
Those policies have not been consistently enforced in certain regions, including several of the states where a reopening process began sooner than in others. Governors of some of these states cite increased coronavirus testing as the reason for the spikes, but that doesn’t fully explain the discrepancies with other states.
There’s still a lot to learn about this virus. It’s possible that open air gatherings, with proper precautions, are less worrisome than being in enclosed spaces with intimate crowds.
But don’t call it a second wave. We’re still in the throes of the first one—more than two million Americans have confirmed COVID-19 cases and more than 113,000 have died to date, per Johns Hopkins. A second wave would happen in the late fall if the current crisis has already abated (a big “if”).
And by the way, readers—please be sure to check out my writeup of our fascinating Brainstorm Health walkup call on the effects of coronavirus on the health care industry ahead of our virtual conference next month. More on that below.
Read on for the day’s news, and see you again next week.
Sy Mukherjee
sayak.mukherjee@fortune.com
@the_sy_guy
DIGITAL HEALTH
The ripple effects of coronavirus on the health industry—including telemedicine. Fortune held a community conversation with prominent health care leaders from across the country in a lead up to our first virtual Brainstorm Health conference in July. Attendees for the wide-ranging discussion included NewYork-Presbyterian hospital president and CEO Steven Corwin, Vivian Lee of Verily Life Sciences, and Komodo Health's Arif Nathoo. One of the main takeaways, among many fascinating observations about how coronavirus will transform the American medical industry, is that telemedicine is now being ingrained into the sector and embraced by patients and doctors alike. (Fortune)
Coronavirus tracing apps get a mixed reaction. "Contact tracing"—the process of following whom a potentially infected coronavirus patient may have interacted with—is a critical part of keeping the outbreak in control. Digital health has a role to play in this since it can, through certain decentralized apps, help people keep tabs on if they've been near those diagnosed with an infection. But there's been a mixed reaction to contact tracing apps developed by companies like Apple and Google over privacy concerns given a lack of national standards. On the flip side, Italy—one of the hardest-hit countries in the pandemic—seems to be warming up to the idea of its own contact tracing programs. (Wall Street Journal)
INDICATIONS
Big Pharma and biotech alike advance their COVID-19 therapies. In the past few weeks (and days), Johnson & Johnson, Moderna, Regeneron, Eli Lilly, AstraZeneca, Amgen, AbbVie, Vir Biotechnology, and GlaxoSmithKline have all announced new advances into COVID-19 therapeutics and vaccines. That's a pretty whopping roster of companies rushing into this space with a whole lot of different methodologies that include using antibody therapies to treat COVID-19 to vaccines which leverage messenger RNA. Some of the most prominent storylines include Johnson & Johnson's Wednesday announcement that it's accelerating its vaccine candidate into early-stage human clinical trials; Moderna's plans to launch a phase 3 clinical trial for its own vaccine, in July, with a dose set at 100 micrograms (for more on that, head over here); GlaxoSmithKline, per a company spokesperson, is advancing a treatment called otilimab to see whether it can block an overreaction of the body's immune system to a COVID-19 case; Regeneron announced Thursday morning that its own combination of two antibody drugs is now in human trials.
THE BIG PICTURE
IMF: The world will need to spend much more to address the pandemic. The International Monetary Fund (IMF) says that countries around the world have already spent $10 trillion combating the coronavirus pandemic and its downstream economic effects—but that isn't nearly enough, per the organization. The group's managing director Kristalina Georgieva says that significant investments will need to be made in order to assist an estimated 100 million people who might be pushed into "extreme poverty" as a result of COVID. (Reuters)
America's Surgeon General: 'George Floyd could have been me.' Surgeon General Jerome Adams, one of the nation's top public health authorities and a black man, tells Politico that the police killing of George Floyd hits home. "I really do think that could have been me," he said. "That could be me who is just seen as a black man and not as the surgeon general of the United States—especially if I'm not wearing a uniform, but I'm casually dressed in my hoodie and tennis shoes and athletic apparel—and that could be me on the side of a road with a knee in my neck." (Politico)
REQUIRED READING
How racism, COVID-19, and air pollution reveal striking patterns of inequality, by Katherine Dunn & Eamon Barrett
More than 44.2 million Americans have filed for unemployment amid the pandemic, by Lance Lambert
How one company manages supply chains for every 'essential' industry, by Emma Hinchliffe











