In the midst of a political season that’s slapped a target on biopharma’s back, public frustration with high drug prices has become palpable. Add to that persistent media coverage of controversial price hikes by companies like Valeant Pharmaceuticals (VRX), and tempers have maintained a slow boil.
Major industry players have started to recognize the existing carte blanche approach to pricing will have to change. Biopharma companies have the freedom to price their medicines as they see fit in the U.S. But an increasing number of healthcare players want to tie drugmakers’ reimbursements to how effective their therapies are for patients.
According to a new report by health analytics firm Avalere, a growing cadre of insurers wants to strike value-based contracts for pricey drugs that treat conditions like hepatitis C, cancer, rheumatoid arthritis, and multiple sclerosis. In a survey of health plans, 63% and 53% said they either had “High” or “Very high” interest in seeking the arrangements for hep C and oncology therapies, respectively.
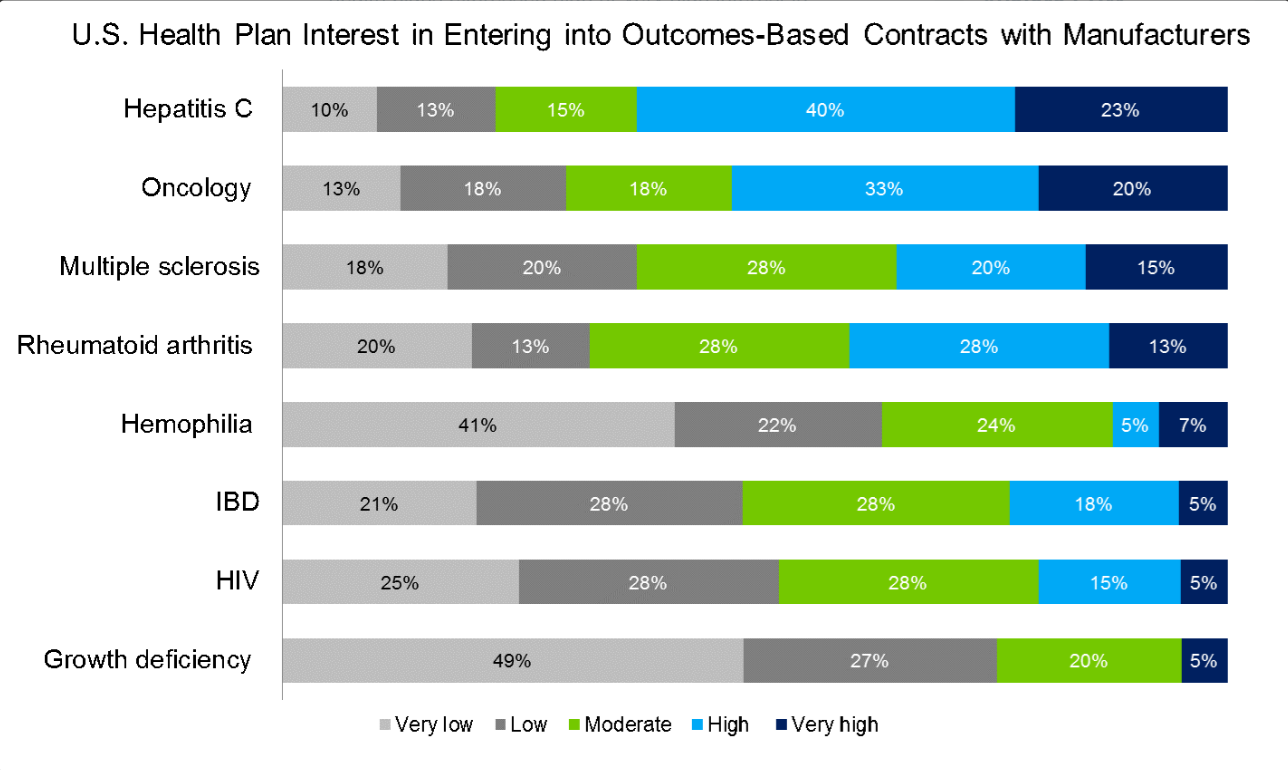
“The growth of outcomes-based contracts between plans and manufacturers is a clear response to the health system’s call for cost-containment without restricting patients’ access to new, breakthrough therapies,” said Dan Mendelson, president at Avalere. “Plans, manufacturers and providers are all looking for ways to reduce cost without comprising patient outcomes and access—these types of contracts are one possible solution.”
And they’re starting to pick up steam. Novartis (NVS) CEO Joe Jimenez has long touted value-based pricing. More recently, Regeneron (REGN) chief Leonard Schleifer also emphasized the importance of patient health outcomes when judging value.
In the coming years, such contracts’ ability to lower health costs to insurers and consumers will be tested. For instance, in May, insurance giant Cigna (CI) struck an outcomes-based deal with Sanofi, its partner Regeneron, and their competitor Amgen (AMGN) for a new class of cholesterol-slashing medications called PCSK9 inhibitors that are far pricier than standard treatments like statins.
The drugs’ list prices stand at about $14,000 per year. But under the arrangement, Cigna won’t have to pay anything close to that if the drugs don’t meet specific cholesterol-reduction benchmarks. The more the treatments do their jobs, the more the insurer will have to shell out to the companies — and, the hope is, the less patients will have to pay for therapies which don’t prove effective.