Five years ago this week, President Obama signed into law the Affordable Care Act, which promised to extend insurance coverage to millions of uninsured Americans and raised fears that doctors would be inundated with new and sicker patients. But it looks like those fears haven’t come to pass, according to a new study.
Doctors across the nation have only seen a slight increase in the number of new patients even as nearly 10 million Americans gained insurance coverage since the launch of ACA-mandated exchanges a year ago, according to a study by health care technology company athenahealth (ATHN) and the Robert Wood Johnson Foundation.
“Amongst other findings and counter to what many predicted, we haven’t seen a swell of new and sicker patients materialize in primary care or across specialty settings,” said Josh Gray, vice president of athenahealth’s research arm. “The findings are fascinating. It’s a front row seat into how policy is translated into care trends, utilization and access across the U.S.”
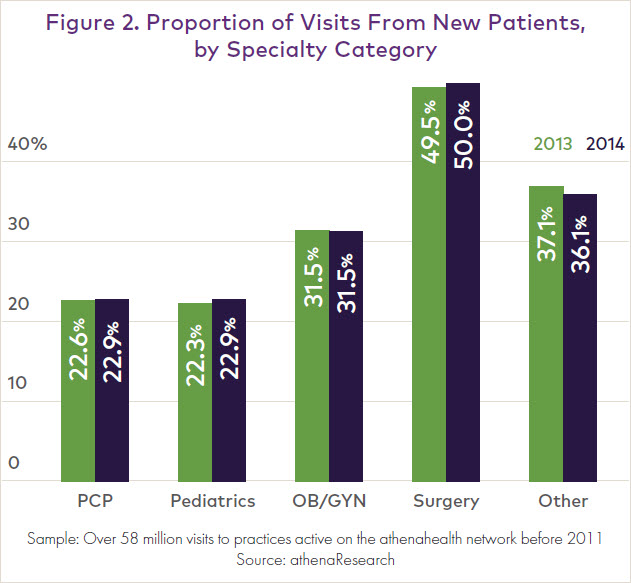
For instance, primary care practitioners had 22.9% of their visits from new patients last year, up from 22.6% in 2013. That is only a 1.3% increase year-over-year, and the new patient influx has been less pronounced for obstetricians/gynecologists and other specialty practitioners.
More importantly, these new patients haven’t been sicker or more complex than previous entrants. A measure of provider effort, which accounts for time, skill and intensity required in different procedures, remained constant while the number of “high complexity” evaluation and management procedures declined to 7.5% last year from 8% in 2013 for all visits.
The study was based on a subset of 16,000 health care providers culled from athenahealth’s database of more than 62,000 medical providers across about 100 specialties nationwide. It used data aggregated from the company’s ambulatory-care software platform, a cloud-based system for managing patient health records, billing and communication. The information represents actual patient-provider encounters rather than less-reliable self-reported responses.
The biggest change for doctors since the implementation of the ACA has been how they are getting paid. As insurance coverage has expanded, the mix of who pays physicians has changed in many states.
Following the Supreme Court’s decision on the constitutionality of the ACA in 2012, states were able to decide if they wanted to increase the number of individuals who qualify for Medicaid. About half of the states decided to do so, while the rest generally maintained their existing approaches to Medicaid eligibility.
In states that expanded Medicaid access, doctors have reported an increase in the proportion of Medicaid patients. Those in states that have stayed with the status quo have had an uptick in the proportion of patients with commercial insurance coverage.
“The providers in these non-expansion states are likely seeing more patients newly insured through the health care marketplaces,” according to the report.
Overall, regardless of state or Medicaid policy, doctors report seeing a lower proportion of uninsured patients year-over-year.
Last year was pivotal for ACA as its central provision on expanding coverage took effect and millions of Americans became newly insured. But much of the law remains in flux as it faces challenges in the Supreme Court and efforts by some members of Congress to revise the law.