For hospitals everywhere it was a crucible—a challenge unlike any that most administrators, doctors, or nurses had ever faced in their lives. It was also, for some, a chance to shine as never before.
In the spring of 2020, as the mysterious coronavirus known as a SARS-CoV-2 began spreading rapidly across the globe and U.S. emergency departments began to face a tsunami of patients with severe respiratory disease, Colorado physician Diana Breyer was carefully, anxiously, getting ready for the wave. Breyer, a pulmonary care doctor at UCHealth Poudre Valley Hospital in Ft. Collins, Colorado, met frequently with the hospital’s respiratory therapy leader, anesthesiologists, nurses, and others, and they gamed out what to do should they experience the same flood of desperately ill patients that New York City hospitals were then witnessing. The team assessed how to double and triple up, if necessary, the number of patients in their ICUs—and then went through practice exercises. They analyzed their supply of ventilators—”the Cadillac vents that could be available to the sickest patients,” as Breyer put it, along with simpler machines that were used just for anesthesia—”and we figured out how we’d use our entire fleet to the top of its scope.”
Poudre Valley, a 270-bed medical center is part of a system of 12 hospitals of varying sizes up and down the Front Range in Colorado, and it managed to avoid a crisis that plagued many other hospital groups during the pandemic—medical supply chains that fell apart at the seams as the pandemic relentlessly strained resources, from oxygen tanks to personal protective equipment (PPE). Breyer, who serves as Chief Quality Officer for Poudre Valley and its Loveland, Colo., affiliate, the Medical Center of the Rockies, chalks up her hospital’s resilience to “a very strong culture or problem-solving”: Administrators, physicians, nurses regularly sit down at the same table to figure out the changing needs of their patient population and how to care for them.
That culture mattered profoundly when the surge of coronavirus cases slammed Poudre Valley Hospital in the fall—when 480 COVID-19 patients suddenly filled its beds, three times the number reached during the hospital’s previous peak in the spring. “I thank goodness for that work we did earlier to prepare,” Breyer says. “Our staff went into the fall surge—I mean, people were tired, there’s no doubt about that. But they also were comfortable in the fact that nobody had gotten sick.” The hospital’s prodigious work on infection control, among so much other advance planning, kept its own workers safe as they cared for others, Breyer says. “Our PPE was working, and our people knew they had been taken care of.”
Spend a moment talking with Breyer and it’s hard not to hear the pride in her voice. The thing you won’t hear is surprise. Maybe that’s because Poudre Valley Hospital has been on IBM Watson Health’s 100 Top Hospitals list for 15 years, the most of any teaching hospital in the country.
This year, Fortune has once again joined forces with IBM Watson Health to rank the very best hospitals and health systems in the country. Crunching the numbers from Medicare cost reports, Medicare Provider Analysis and Review (MEDPAR) data, and data from the Centers for Medicare & Medicaid Services (CMS) Hospital Compare website, IBM researchers evaluated 2,675 short-term, acute care, non-federal U.S. hospitals on various performance indicators in four main categories: clinical outcomes, operational efficiency, patient experience, and financial health. (For a separate ranking on health systems, the team also evaluated 324 such health organizations along with 2,522 hospitals that are members of health systems—please see our complete methodology here.)
And this year, we added a crucial fifth category: how hospitals engaged with the goal of improving the wellbeing of the entire community outside their walls.
This “community health” measure, in large part inspired by the work and passion of Bernard J. Tyson, the legendary CEO of Kaiser Permanente who died in November 2019, signals a radical departure in the way hospitals have long been judged—holding medical centers accountable for their central role in the communities in which they operate. Measuring such involvement isn’t easy—but we think we’ve made a good start in this year’s inaugural effort. IBM Watson Health and Fortune teamed up with researchers at the Johns Hopkins Center for Health Equity and Bloomberg American Health Initiative at Johns Hopkins Bloomberg School of Public Health to survey three fundamental components of hospital-community engagement.
First, we looked at how each medical center acts to protect patients both in the hospital and after they’ve been discharged: Does the hospital screen for drug and alcohol abuse and domestic violence, for instance? Does it help patients quit smoking, provide breastfeeding training to new mothers, help reduce falls among older people in the community?
Then we examined how the hospital partners with other community-based programs—from those that offer home visits to the elderly to efforts to bring local greenmarkets to neighborhood “food deserts.” “We looked to see if they’d engaged in evidence-based initiatives like the Diabetes Prevention Program or some of the hypertension screening and prevention programs that have been tested in barbershops and other kinds of community locations,” says physician Rachel Thornton, an associate professor at John Hopkins School of Medicine who helped develop our ranking’s community health measures. “We wanted to see how hospitals are partnering to get community health workers, health navigators, and lay health experts out into the community to help people engage with the hospital when they do need health care,” says Thornton, who is also the Associate Director for Policy at the Johns Hopkins Center for Health Equity.
And last, we gave hospitals their own check-up as “anchor institutions,” given that many are also the largest employers in the area: How do they treat their own workers and suppliers; how do they interact with patients who have trouble paying their bills? Are hospital workers and patients of different means and backgrounds treated equitably?
“We want the hospital industry to help support a healthier and more just community,” says Joshua Sharfstein, a physician and Vice Dean for Public Health Practice and Community Engagement at the Johns Hopkins Bloomberg School of Public Health. “And that is the fundamental shift here. That’s also what makes this quite a challenging set of measures to put in place. “We’re saying, in effect, ‘Look, you can have satisfied customers. You can give your patients exactly the right medicine when they come in and offer high-quality care, and you’re still not fully doing your full job as a hospital if there’s this fundamental problem in the community—if, for instance, people are dying of drug overdoses on the street outside.’ There’s something kind of radical about that idea.”
So why embrace such a revolutionary concept? The simple answer is that what truly keeps people healthy goes well beyond medical intervention—and hospitals not only can be a part of providing these critical components of wellbeing, they also ought to be. “Hospitals can help keep people being healthy, first of all, by making sure they offer the services that really keep people healthy,” says Sharfstein, who earned widespread plaudits when he served as Secretary of the Maryland Department of Health and Mental Hygiene and worked to rethink the entire compensation structure for that state’s hospitals.
“Health is not just limited to what happens within the health care system,” agrees Irene Dankwa-Mullen, Deputy Chief Health Officer and Chief Health Equity Officer at IBM Watson Health. “During the pandemic, we really got to understand how social factors and economic determinants contribute to health and we have so much to learn from what hospitals are already doing in this regard. If anything, the past year has been a call for action to learn even more.”
We agree. And what better way to start learning than seeing why the elite crowd of hospitals below stands out from the pack.—Clifton Leaf, Editor-in-Chief, Fortune




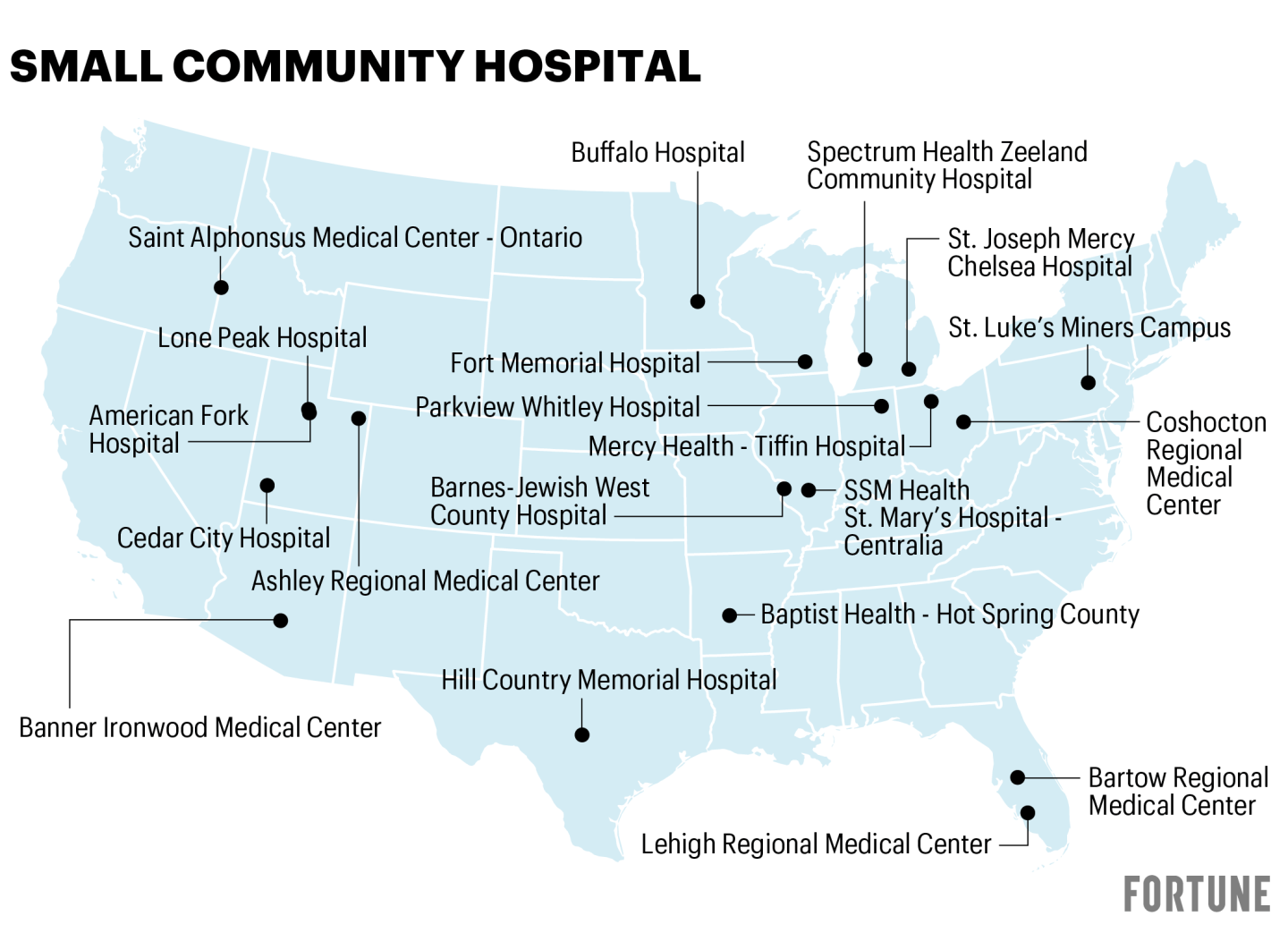

Fortune/IBM Watson Health 100 Top Hospitals

IBM, Watson Health and 100 Top Hospitals are registered trademarks of International Business Machines Corporation in the United States and other countries. FORTUNE is a trademark of Fortune Media IP Limited; registered in the U.S. and other countries.












