Soon after the first shipments of Pfizer/BioNTech’s COVID-19 vaccine began arriving in December, health care workers and administrators discovered a precious opportunity. Though the vaccine vials were labeled as containing five doses, experienced health workers found that they could sometimes extract a sixth dose, effectively expanding their vaccine supply by 20%.
But Pfizer’s extra dose comes with a catch. To consistently deliver it, health workers would ideally be using specialized equipment known as a low dead space syringe, or LDS syringe. While standard syringes retain a small amount of medicine after an injection, LDS syringes are designed to push nearly all of the liquid into a patient’s arm. That waste reduction is enough to turn five doses into six.
The problem is that LDS syringes are normally a niche product, and there are not enough available, either in the U.S. or worldwide, to administer all of those extra doses over coming weeks and months. Most producers of the syringes have said they cannot expand production capacity.
The Biden administration says it has contracted for an adequate supply of syringes to deliver all of the Pfizer doses. That’s possible because the supply of LDS syringes is being supplemented with other syringes that the White House and Pfizer say are workable alternatives.
But vaccine administrators and experts say those alternatives are not consistently extracting the sixth dose. Public health leaders say that poses a risk to a steady U.S. vaccine supply. And as threats to the miraculous sixth dose appear to rise, the U.S. is still paying Pfizer for it—whether it winds up in anyone’s arm or not.
A lifesaving surprise
For the most agile vaccine administrators, the extra Pfizer dose was a godsend.
“We very quickly got the information from the CDC that we could use that sixth dose,” says Krista Capehart, a pharmacist and member of the West Virginia COVID task force. “And most of our pharmacists were getting it because that’s what they do.”
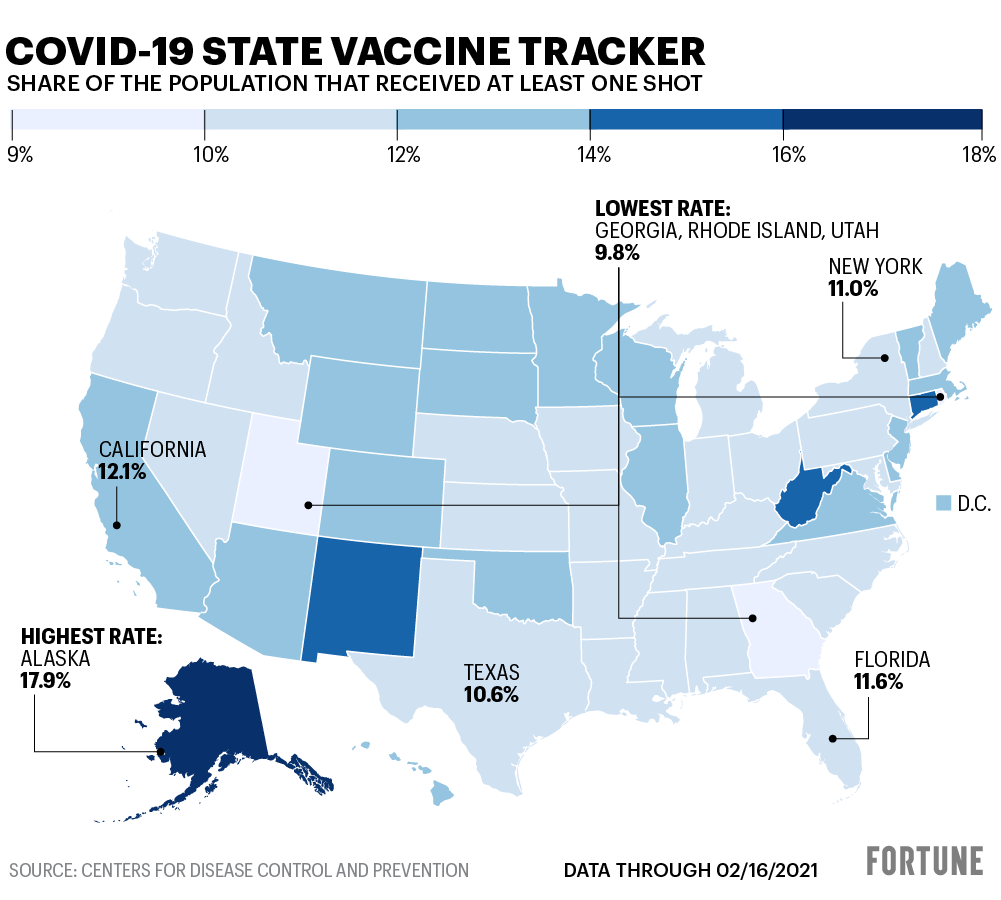
Capehart has had a central role in managing vaccine distribution in West Virginia, which has been widely praised for its effective rollout. West Virginia currently has one of the highest first-dose vaccination rates in the country, at 14%, and Capehart says early recognition of the potential extra dose played a role in that success.
The extra sixth Pfizer dose has continued to help accelerate vaccinations across the U.S. and the world. In late January, Pfizer announced that the extra dose would enable it to deliver 200 million doses to the U.S. by the end of May, two months ahead of schedule. The Biden administration has announced a more than 20% expansion of the U.S. weekly vaccine supply in recent weeks, and about one-third of that increase is thanks to the extra Pfizer dose, according to a White House official.
That expanded supply could ultimately save tens of thousands of American lives, especially as the new and more infectious U.K. variant of the SARS-CoV-2 virus, which responds well to current vaccines, gains a foothold in the U.S.
But the shortage of low dead space syringes threatens that momentum. In normal times, LDS syringes are used to get the most out of expensive cancer medications or in needle exchange programs to reduce disease transmission among IV drug users. Producers have been unable to scale up from that small base to meet exploding demand driven by vaccinations. The U.S. government has contracted with U.S. syringe maker BD for 40 million of those syringes, but BD has signaled it is unable to further expand its production capacity. A White House official told Fortune that the bulk of the federal supply of LDS syringes is coming from Retractable Technologies Inc. (RTI) but did not specify how many the contract included.
LDS syringes are also manufactured in China, but those sources, too, are already at capacity, according to recent reporting by the Global Times. One Chinese producer, Shanghai Kindly Enterprise Development Group, said that new syringe orders are now in a queue and will not be fulfilled until August.
To help its supply go further, the White House COVID team announced on Feb. 1 that while 80% of the syringes being packed with Pfizer vaccination kits are the preferred LDS type, 20% are alternatives also capable of extracting all six doses. Thirty-five different combinations of syringe and needle, determined with involvement from both Pfizer and the federal government, fall in that category of workable alternatives.
But vaccinators on the ground are already seeing a more troubling reality. According to Capehart, recent vaccine shipments have contained “this mishmash of syringes…Particularly with Pfizer, we were definitely short” of syringes effective at extracting all six doses. Vaccine administrators in states including New Jersey have reported a similar shortfall of appropriate needles in Pfizer kits, despite assurances from the Biden administration.
As a result, Capehart says that in West Virginia, “we’re certainly not seeing the extra doses we were at the beginning.”
The six-dose challenge
That’s particularly worrying because on Jan. 6, the extra Pfizer dose was transformed from a blessing into something more complicated. The FDA revised its emergency use authorization to make it official that each vial contained six doses. This revision meant that, as long as acceptable syringes were provided, Pfizer could charge for the sixth dose, changing it from a bonus to an expectation.
But even if LDS syringes were plentiful, experts say the six-dose expectation may not reflect a more complex reality. Crucially, they say, the “surprise” sixth dose was actually not a surprise: All vaccines are delivered with some degree of overfill—and for good reason.
“One of the most important principles of engineering is you need to have some sort of redundancy,” says Tinglong Dai, a professor of health care operations at Johns Hopkins. “There’s always going to be some sort of waste.”
Redundancy is important because the volumes involved are so tiny. After preparation, each Pfizer vial amounts to just 2.25 milliliters of liquid. Turning that into six doses means a much smaller margin of error as vaccinators draw each 0.3 ml vaccine dose—roughly the length of an adult’s pinky nail—in a syringe.
“[Vaccinators] are telling me for the most part they’re getting the sixth dose,” says Dai. “But…it’s not a guaranteed thing, even with the low dead space syringes. It’s a matter of training.”
Pressure to get that dose is heightened now that Pfizer can count it toward its contract with the U.S. government. That contract promised 200 million doses, not a specific number of vials, and Pfizer announced in January that it would ship fewer vials to the U.S., though at a faster pace, to account for the extra doses.
Similar changes have led to controversy in the EU, where Pfizer has been accused of charging customers for the sixth dose, even when the needles required to extract all six doses can’t be found. Health officials in Germany, France, Italy, and elsewhere have warned that the labeling revision could actually reduce the rate of vaccination.
By providing an inconsistent mix of LDS and “equivalent” syringes with the Pfizer vaccine, while still assuming each vial will deliver six doses, the Biden administration risks re-creating the same situation in the U.S.
Missed opportunities
The shortage of ideal syringes appears to be the product of a lack of coordination between federal authorities, Pfizer, and syringe manufacturers dating back as far as early 2020. And specialized LDS syringes are not the only cause for concern.
While the extra dose came as a surprise to vaccinators in the field, Pfizer had reportedly been testing methods for extracting the extra dose since August 2020. But Pfizer did not broach the topic of the sixth dose with the FDA until December. While it wouldn’t have necessarily eliminated bottlenecks, better communication would have given more time for a ramp-up in production of LDS syringes, according to experts interviewed by the Washington Post.
Broader syringe supply issues may, in part, be due to inaction by the Trump administration. Rick Bright, the former director of the HHS Biomedical Advanced Research and Development Authority (BARDA), alleged in a whistleblower complaint that he repeatedly warned about a potential shortage of syringes of all kinds as early as March 2020. Bright’s complaint alleges not only that his warnings were dismissed by leadership including then-HHS Secretary Alex Azar, but also that Bright was effectively demoted against his will in what he claims was retaliation for his persistence on this and related issues. Bright resigned soon after.
There are signs that supply issues are having an impact beyond the Pfizer vaccine. On Jan. 29, Capehart says, packages of Moderna vaccine sent to West Virginia included 1.5-inch 23-gauge needles, much larger than standard vaccination needles.
“A 23-gauge needle is like a nail going into your arm,” Capehart says.
But worse than the discomfort is the fact that the needles couldn’t extract all 10 doses in a Moderna vial. Capehart says her vaccinators were able to get only eight doses from each vial with the needles, forcing her to replace the needles from the state’s own reserves.
Looming disruption
If there is a shortfall of syringes capable of reliably extracting all six Pfizer doses, “you’re going to see appointments canceled,” says Amesh Adalja, a senior scholar at the Johns Hopkins Center for Health Security. “Then they’re going to have to adjust the number of doses down, and the timeline will adjust. That’s just going to further slow down the vaccine rollout, and further complicate things.”
In its Jan. 21 COVID-19 response strategy document, the Biden administration said it plans to make use of the Defense Production Act to increase the supply of low dead space syringes and other needed equipment. But it’s unclear whether the DPA can accomplish that. The law applies only to domestic U.S. producers, and the only manufacturer who produces LDS syringes in the U.S., BD, has said it has no capability to increase its output.
Manufacturers capable of retooling from related products can be compelled to produce emergency supplies under the DPA, as when Donald Trump ordered GM to make ventilators last fall. But after decades of offshoring, finding U.S. manufacturing facilities capable of producing precision medical devices isn’t easy. Nearly a month after releasing the strategy document, the Biden administration has yet to invoke the DPA to expand syringe production.
Meanwhile, there is little market incentive to build new factories or otherwise invest in producing more LDS syringes. Despite huge demand over the next few months, there’s no reason to believe the need will last much beyond that. Biden officials are signaling that vaccinations will be widely available in the U.S. as soon as April, partly thanks to the expected approval of more types of vaccine, such as Johnson & Johnson’s. That could mean reduced pressure to extract the sixth Pfizer dose and a rapid reduction in demand for LDS syringes.
Pfizer, for its part, says it is “helping countries secure access to the necessary equipment” to secure all six doses. But it has not yet signaled that it will directly involve itself in efforts to increase syringe supplies—despite having arguably the strongest incentives of any stakeholder.
“An LDS syringe will probably cost you 10 cents,” says Tinglong Dai. “But if you squeeze out another dose, [Pfizer] can charge the government $20. Wow, this is probably the highest return on investment I’ve ever heard of in the medical industry.”











